Intraosseous Access Needles in Pediatric Emergencies And Manufacturer Expertise For 2026
Apr 16, 2026
Top 10 Applications of Intraosseous Access Needles in Pediatric Emergencies and Manufacturer Expertise for 2026
In 2026, the application of intraosseous (IO) access needles in pediatric emergencies has evolved from a last resort to a first-line technique, becoming an indispensable lifeline in the resuscitation of critically ill children. The unique physiological and anatomical characteristics of children impose specific requirements on IO devices. Leading global manufacturers have developed specialized product lines and solutions tailored to the distinct needs of pediatric patients.
Physiological Basis of Pediatric IO Access
The pediatric bone marrow cavity contains a rich network of vascular sinuses directly connected to the systemic circulation. Drugs and fluids administered via IO access rapidly enter the central circulation. Studies indicate that the peak concentration time and bioavailability of drugs administered through the proximal tibial IO route are comparable to central venous access, significantly outperforming peripheral venous access. This physiological characteristic gives IO access unique value in pediatric emergencies.
The developmental characteristics of children's bones dictate the specific design of IO devices:
Thinner Cortex, Higher Resilience: Requires precisely controlled insertion force.
Presence of Growth Plates: Necessitates cautious site selection to prevent damage that could impair bone development.
Relatively Larger Marrow Cavity: Allows for the use of smaller diameter needles.
Variable Bone Size: Requires a graded system of products that accommodate different ages.
Technical Features of Pediatric-Specific IO Devices
IO devices designed for pediatric patients feature:
Graduated Diameter Systems: Offering choices based on age, weight, and insertion site (e.g., 18G for neonates/infants, 16–18G for toddlers, 15–16G for school-age children, and adult sizes for adolescents).
Optimized Length Design: Adapting to anatomy (e.g., 15–25mm for proximal tibia, 25–45mm for humerus).
Visual Depth Markings: Assisting operators in precisely controlling depth to prevent posterior cortex penetration or growth plate injury.
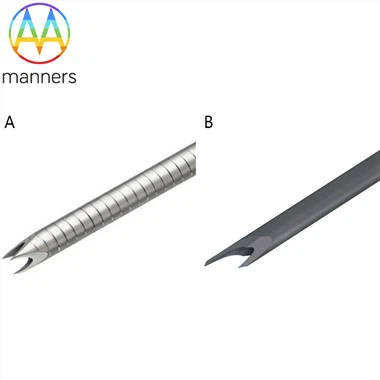
Low-Resistance Tips: Reducing the force required for insertion and lowering the risk of bone fracture.
Safety Locking Mechanisms: Preventing accidental needle movement and maintaining stability.
Teleflex's Pediatric EZ-IO system is specifically engineered for children, offering needle gauges from 15G to 18G and lengths from 15mm to 45mm, covering newborns to adolescents. Its intelligent driver automatically detects bone density and adjusts drilling parameters to ensure safety.
Critical Role in Neonatal Resuscitation
In neonatal resuscitation, when umbilical venous access is unavailable or fails, the proximal tibial IO route becomes the primary alternative. The proximal tibia in neonates has rich blood supply and a high success rate with minimal complications. IO access provides a rapid conduit for critical drugs like epinephrine, volume expanders, and sodium bicarbonate.
IO needles designed specifically for neonates feature smaller diameters (typically 18–20G), shorter lengths (10–15mm), and sharper tip angles. The puncture site is the flat medial area of the proximal tibia to avoid growth plates. Precise depth control is paramount to prevent penetrating the posterior cortex.
PerSys Medical's neonatal IO system integrates a dedicated stabilizer and depth limiter to ensure precision and control. The system's compatible micro-infusion sets allow for accurate flow rates, adhering to neonatal fluid management requirements.
Comprehensive Application in Pediatric Critical Illness
IO access plays a vital role in various pediatric critical conditions:
Status Epilepticus: Ensures rapid delivery of anticonvulsants to the central nervous system.
Severe Septic Shock: Provides a reliable option for rapid antibiotic administration and fluid resuscitation when venous access is difficult.
Diabetic Ketoacidosis: Offers a route for insulin therapy and fluid replacement in severely dehydrated children.
Congenital Heart Disease: Avoids the stress response associated with repeated peripheral punctures in children with compromised cardiac function.
Trauma with Hemorrhagic Shock: Provides a lifeline for rapid fluid resuscitation.
Smiths Medical's pediatric IO solution is optimized for diverse scenarios, featuring rapid infusion sets capable of delivering 20 ml/kg of fluid within 3 minutes to meet shock resuscitation demands. A built-in dose calculator adjusts infusion rates based on the child's weight, reducing medication errors.
Considerations for Special Pediatric Populations
Certain pediatric groups have unique IO requirements:
Obese Children: Deep subcutaneous tissue obscures landmarks; ultrasound-guided IO is essential for success.
Bone Dysplasia (e.g., Osteogenesis Imperfecta): Requires extremely cautious technique and specialized needles.
Bleeding Disorders (e.g., Hemophilia): Risk-benefit ratios must be carefully evaluated, with IO placement potentially deferred until factor replacement is administered.
Malignancy: When venous access is exhausted, IO provides a temporary route for emergency treatment.
IO devices for these special populations often feature adjustable insertion parameters, varied tip designs, and real-time pressure monitoring. Thorough pre-procedural assessment and personalized planning are crucial.
Operational Techniques and Training Systems
Pediatric IO insertion demands high technical proficiency, making systematic training essential:
Simulation Training: Uses pediatric-specific bone models to realistically simulate skeletal characteristics across ages.
Virtual Reality (VR) Platforms: Simulates diverse pediatric emergency scenarios to enhance clinical decision-making.
Competency Certification: Ensures operators master the unique skills required for pediatric IO.
Continuous Quality Improvement (CQI): Optimizes pediatric IO outcomes through data collection and analysis.
Dedicated pediatric IO training programs emphasize age-specific anatomy, growth plate protection principles, complication management, psychological soothing techniques, and family communication strategies. Child-friendly training materials help reduce anxiety for both staff and patients.
Complication Prevention and Management
Although the incidence of complications with pediatric IO is low, vigilance is required:
Infection Risk: Managed through strict aseptic technique and timely removal.
Fracture Risk: Prevented by using correct technique and appropriate needle selection.
Growth Plate Injury: Avoided by correct site selection and depth control.
Extravasation: Prevented by secure fixation and appropriate infusion pressure.
Fat Embolism: Rare but serious; prevented by standardized operation and monitoring.
Modern pediatric IO devices integrate multiple safety features: real-time pressure monitoring for early warning, stable fixation devices, biocompatible coatings to reduce tissue reaction, and visualization systems for guidance.
Future Development Directions
The future of pediatric IO technology includes:
Further Refinement of Age-Specific Systems: Covering the full spectrum from premature infants to adolescents.
Smart Puncture Guidance: Integrating ultrasound and optical navigation for enhanced precision.
Bioabsorbable IO Needles: Gradually degrading after treatment to avoid secondary removal procedures.
Wireless Monitoring Systems: Tracking the functional status of the IO access in real-time to detect early complications.
Home Care IO Devices: Providing treatment options for children with chronic illnesses.
With the advancement of pediatric emergency medicine and IO technology, intraosseous access needles will play an increasingly critical role in rescuing critically ill children. Manufacturers are driving innovation and clinical collaboration to develop better pediatric solutions.
Leading global pediatric medical organizations are promoting the standardized application of IO technology in pediatric emergencies by establishing age-specific guidelines and quality standards. These efforts will further enhance the safety and efficacy of pediatric IO access, ultimately improving the prognosis of critically ill children.