Ultrasound-Guided Nerve Blocks – A Must-Read for Beginners
Jul 22, 2024
What is the hottest technique in the field of anesthesia today?
Everyone may have their own answer, but one of the most widely agreed-upon answers is: "ultrasound."
Thanks to the promotion by anesthesia professional associations, ultrasound-guided nerve block techniques are increasingly accepted in clinical practice, and many new techniques are constantly emerging.
However, due to various factors, some practitioners may just be starting to learn about ultrasound. Therefore, there is a great thirst for ultrasound knowledge in many places. So, how can we quickly become proficient from a beginner level?
The answer is: in-depth study of anatomy!
Ⅰ Importance of Anatomical Knowledge
Although ultrasound is an excellent clinical tool, knowing how to use ultrasound does not automatically mean we can identify the anatomical location of nerves. Instead, a thorough understanding of anatomical knowledge is essential to accurately interpret ultrasound images.
Let's take a look at the image below.

See, if you are not familiar with anatomy, can you quickly and accurately locate the nerve on the ultrasound image? I don't think so. However, if we remember the anatomical structure diagram below, it will be much easier to interpret the ultrasound image above!

Therefore, in-depth study of anatomical structures is the correct path for learning ultrasound-guided nerve blocks.
Ⅱ Learning Spatial Anatomy
First of all, learning ultrasound-guided nerve blocks involves understanding the spatial anatomy of nerves, blood vessels, muscles, and bones.
In the past, when performing "blind" nerve blocks, we focused more on surface anatomical landmarks. For example, for interscalene blocks, we would palpate the groove, insert the needle, inject if there was paresthesia, and adjust the needle direction if there wasn't. In other words, we only located the "groove" without precisely locating the nerve.
Conversely, when performing nerve blocks under ultrasound guidance, the first step is to locate the nerve.
However, this is often the most easily overlooked aspect for beginners!
When we first started learning ultrasound, we would frequently ask, "Teacher, is this round, dark spot the nerve?" We hoped for a "Yes" with eager anticipation.
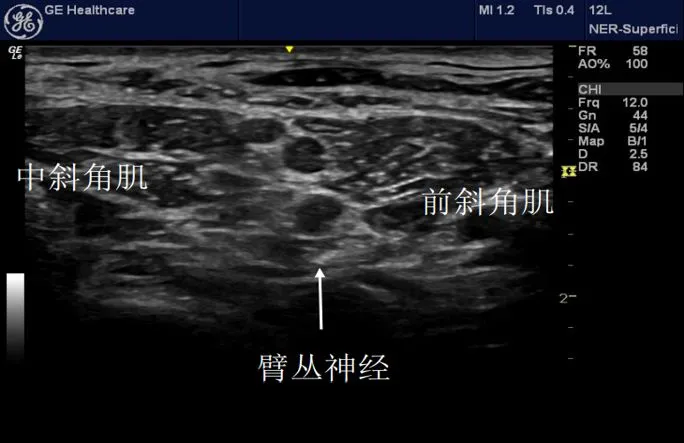
But after studying ultrasound for a while, you'll realize that's not the right approach. Due to the limitations of ultrasound resolution, it is sometimes difficult to confirm nerves based solely on ultrasound images.
Ⅲ Combining Anatomy and Ultrasound
This means that during ultrasound-guided nerve blocks, we do not only focus on the nerve but also consider the course of the nerve and its relationship with muscles, bones, and blood vessels to ultimately determine its location.
For example, in clinical practice, when performing an interscalene brachial plexus block, we identify the anterior scalene muscle, middle scalene muscle, transverse processes of the vertebrae, carotid artery, vertebral artery, and phrenic nerve. By understanding their spatial relationships, we can determine the exact location of each nerve and then proceed with the needle insertion and medication injection.

The advantage of this method is that we can be 100% sure of the target nerve. Additionally, having a clear understanding of the anatomical structures allows us to handle a variety of patients in clinical practice.
Ⅳ Utilizing New Ultrasound Technologies
Of course, besides having a thorough understanding of anatomical structures, we also need to utilize some new ultrasound techniques that enhance imaging, accurately identify nerve courses, and injection sites, thereby increasing the success rate of punctures and reducing complications. For example:
GE Clinical Ultrasound Needle Gain Enhancement Technology:
A near-vertical incident angle enhances needle visibility during ultrasound-guided puncture procedures. Adjustable gain and six levels of beam deflection angles make the needle, especially the tip, clearer and easier to observe under ultrasound, accurately identifying the nerve course and injection site, thereby improving the success rate of nerve blocks.


The image below shows a clinical transversus abdominis plane (TAP) block. Under ultrasound, the three-layer structure of the abdominal wall is clearly visible. Adjusting to the Needle Gain mode, the puncture needle's course, including the needle tip and ideal puncture point, can be clearly displayed. After injection, the distribution of the local anesthetic can be accurately identified.

Ⅴ In-Depth Study of Nerve Innervation
Secondly, in the process of learning ultrasound-guided nerve blocks, we must also study the innervation areas of various nerves more deeply.
Compared to traditional nerve blocks, the advantage of ultrasound visualization is its precision. This precision allows for more selective nerve blocks, reducing the amount of local anesthetic used and preventing complications. Therefore, we need to have a more accurate understanding of the nerve supply in various areas.
For instance, previously, for shoulder surgery analgesia, interscalene brachial plexus blocks were commonly chosen. Although effective, even with ultrasound guidance, this method could still inadvertently block the phrenic nerve, posing risks for patients with poor respiratory function.
By studying the innervation of the shoulder joint in more detail, we find that it is mainly supplied by the axillary nerve and the suprascapular nerve. Therefore, under ultrasound guidance, we can selectively block the axillary nerve and suprascapular nerve.


However, for beginners, mastering complex nerve anatomy and the clinical application of ultrasound can be quite challenging. With the development of new technologies, various ultrasound tools are being applied in clinical practice, providing convenience and enhancing safety.
GE Ultrasound Patent Technologies:
- Fusion Follow-up Intelligent Tracking – Follow-up Assistant:
- This technology automatically restores previous scan parameters, extracts high-echo structures from previous scans as navigation markers, and quickly guides the operator to match the previous scan plane. This helps beginners quickly and accurately find the scan plane and assists experienced practitioners in verifying scan consistency, facilitating patient progress tracking and comparison.


Ⅵ Conclusion
Like all clinical procedures, ultrasound-guided nerve blocks require continuous learning and practice. This includes fundamental anatomical knowledge, ultrasound probe usage, needle positioning, trying new techniques, and understanding surgical approaches. There are no shortcuts to becoming proficient, only dedication and practice.







